National Breastfeeding Month and The Global Big Latch On!August is National Breastfeeding Month, with the first week designated as World Breastfeeding Week. During WBW, Big Latch Ons are held at registered locations around the world. The first Big Latch On had 2 participating countries ... in 2015 there were 28! The Big Latch on is an advocacy event focusing on peer support and community development, aiming to strengthen overall support for breastfeeding and to improve the health of children and women globally. Water Street Big Latch OnThis year on August 5th, I had the opportunity to host a local Big Latch On at the Water Street Park in Hellertown, PA. Our sponsor was Children's HealthCare/The Lehigh Valley Breastfeeding Center. They are an amazing group of pediatricians, lactation consultants, and other practitioners located in Allentown, PA. Jodi Chandler Photography generously donated her time to photograph the Big Latch On - checkout the slideshow below for some photos! The morning of the event we had over 100 registered participants! Our youngest participant was 8 days old, and our oldest was 35.5 months! Our official numbers are below: We couldn't have done it without you...
do it again!
1 Comment
When discussing their birth preferences prenatally, I always try to get the point across to my clients that even the best laid plans may change. One particular client of mine was really interested in having a drug-free natural birth this time around, having had an induction and epidural with her first birth. When her doctor suggested an induction around 39 weeks for medical reasons, she began the process of researching different induction techniques and talking to her OBGYNS on their methods. Because she was already dilated some, they decided a membrane sweep would be a good place to start. A membrane sweep is done by the care provider carefully separating the amniotic sac from the cervix using their fingers. Sometimes this is enough to kickstart a woman's labor without resorting to Pitocin. The membrane sweep did cause some contractions for her, but did not start active labor. A few days later another sweep was done, which did eventually get things moving. To get her contractions stronger and closer together, she used an electric breast pump on and off. This helps release hormones that makes the contractions more effective. For medical reasons, her OBGYN wanted the baby delivered as soon as possible, so she was instructed to head to the hospital as soon as her contractions picked up. Upon admission, she was 4 cm dilated. After laboring in the Jacuzzi for a little bit, and feeling completely overwhelmed by her contractions (which were one on top of each other), she grappled with the decision to get an epidural. Her plan all along has been to have a drug free birth, but she was open to the idea of pain medications, if she felt them necessary. Now 7cm along, and having had a discussion with her nurse, she decided on narcotic pain relief - in this case Stadol was used. Narcotics help take the edge off, but don't completely take away the pain of labor. It was apparent to everyone that she was much more calm and handling her contractions differently than before after receiving Stadol. In what seemed like an instant, she had the urge to push. We all knew this baby would be big, (her son was over 8 pounds) so alternative pushing positions were discussed prenatally. Alternative pushing positions are those that avoid laying on the back, and help create a wider outlet for baby to move down the birth canal. We did some rebozo work together, and so did her nurse. Her nurse was amazingly supportive. She used the squat bar, and semi reclined pushing. Pushing like this helps open up the pelvis in perfect alignment to bring the baby down & out. After pushing for only several minutes, Alexandra Raelyn was born at 8:56pm and was 8 pounds 10 ounces and 21 inches long. She came out fast and furious! She was welcomed earthside by her father, and mom's best friend who was expecting her own baby, any day! Photo credits to Emeigh Photography.
My clients labor began with her water breaking in the middle of the night. Very irregular contractions followed, and after several hours with no changes, it became necessary for her doctor to augment in an effort to get things moving along. Opting for a drug free labor, she walked, used the jacuzzi, bounced on the birth ball, and sang and danced to everything from Beyoncé, to Prince and Nirvana. Using those coping mechanisms helped to keep her mind focused on riding the waves of contractions. They remained irregular after many hours, despite high doses of medication. Her doctor laid out a few choices for them to discuss and ultimately they decided to go ahead and birth the baby via ceserean section. They were very excited and anxious to meet their baby! Most of her original birth preferences were able to be carried out, which was appreciated greatly - including skin to skin, and delayed cord clamping in the OR. This is now standard of care, as the hospital works towards their baby friendly initiative certification. Hunter Marie weighed 6 pounds 7 ounces, and was 20 inches long. Welcoming her earthside alongside her parents was her maternal grandmother - who hails all the way from Chicago! I got the text at 7:41 on Friday evening and by midnight we were in triage getting checked for admission to L&D. S was admitted around 4cm dilated and was urged by the nurse to walk the halls to get things moving. Instead, she felt comfort from taking a warm shower. While in the shower she made up her mind on getting an epidural. The decision came from the fact the she was very tired, and she figured the epidural would help her sleep. Her birth preference had been to give birth without medication, so we talked about waiting until after she was checked again, to make her final decision. S was focused inward during her contractions; blowing each one out of the way, in an almost meditative state whilst waiting for the next. I thought she handled the discomfort of labor like a birthing goddess! S got out of the shower after a while and began another 20 minutes or so of monitoring the baby. The nurses like to make sure the baby's heart tones are normal every so often. After this round of monitoring, and feeling intense pressure (all while waiting for anesthesia to be called for her epidural), she asked to be checked again and was 9cm. No time for sleep :) S's Doctor thought if her water was broken, she'd have a baby in no time. S agreed, and within a few minutes, she was actually involuntarily pushing her baby out! Amara's cord was short, so S opted against delayed cord clamping, in favor of immediate skin-to-skin. Baby Amara was born at 3:40am after only 2-3 pushes. She was 7 pounds 6 ounces and 19.5" long. My job as a doula is to support my clients desires for her perfect birth - whatever that be. If it strays from the original "birth plan" by her choice, than so be it. In many instances, a mother just needs a little encouragement to keep going and work towards her original goal - in S's situation, she was tired and thought she had many more hours to go - so she asked for an epidural. Her body and baby were working so well together, her labor progressed at a fast pace and she ended up not needing one! Baby Amara joined her parents and Big Brother Declan at home just in time to celebrate their wedding anniversary!
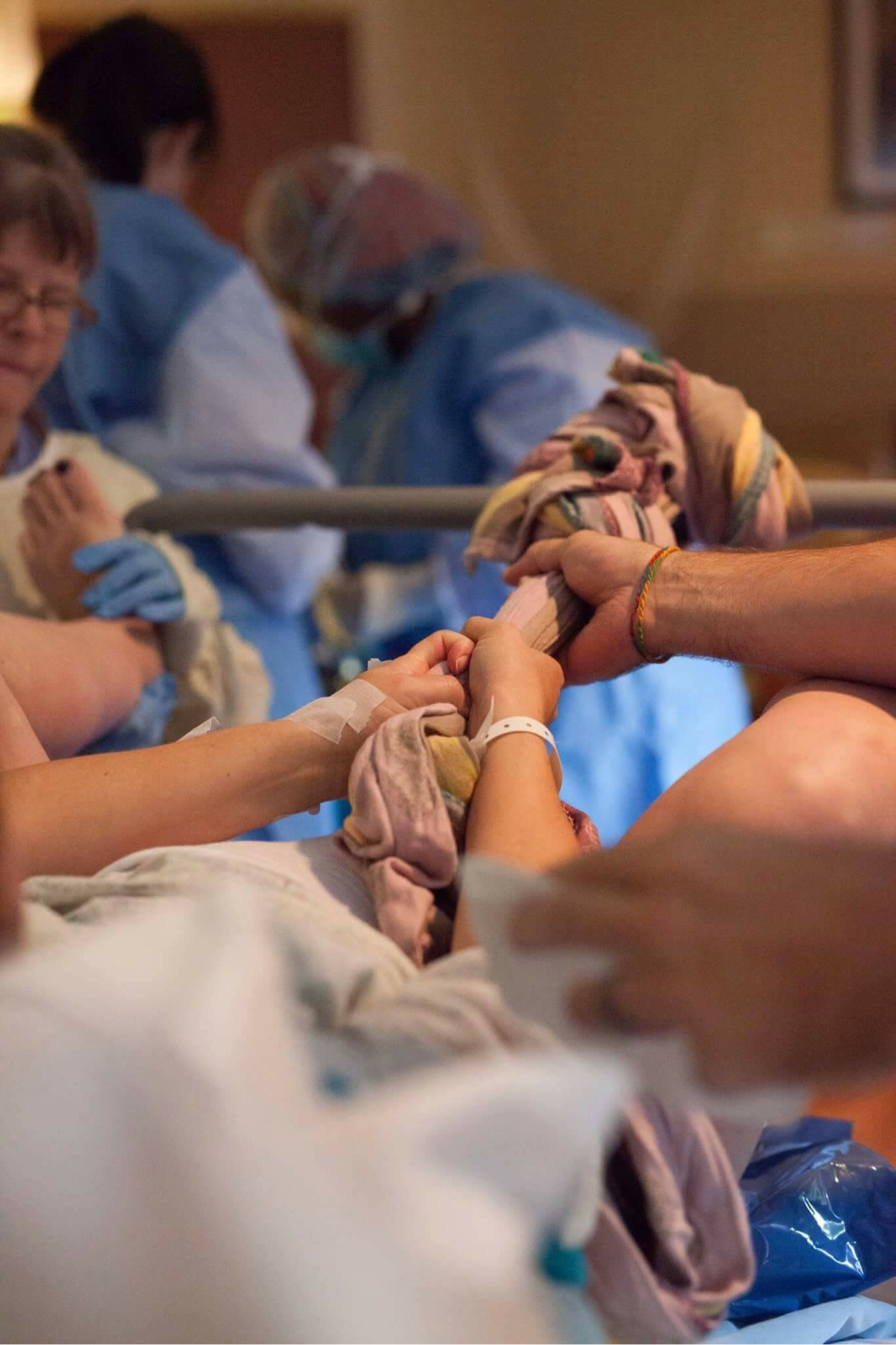
Chiropractic care refers to a form of healthcare that does not use drugs or surgery to achieve and maintain optimal health. Instead, chiropractors offer modalities such a as joint manipulation, adjustments, rehabilitation, and nutritional therapies. Many soon-to-be moms have heard of the Webster Technique. But what exactly is The Webster Technique? The Webster Technique was developed in 1978 by Dr. Larry Webster as a specific adjustment for pregnant women. The purpose is to ease the cause of intrauterine constraint. The Webster Technique is often described as a “breech turning technique”. This is not accurate. When the Webster Technique is done, no forces are placed on the baby to try and turn the baby. The purpose of The Webster Technique is to get the baby to turn by itself. What is intrauterine constraint? Intrauterine constraint is defined as forces external to the developing fetus that obstructs the normal movement of the fetus. Intrauterine constraint can prevent the developing fetus from attaining a head down vertex position thus resulting in a breech presentation and most likely a cesarean section. Today, nearly 13% of all cesarean deliveries performed are due to breech presentation. The Webster Technique is a specialized chiropractic adjustment to help realign the pelvis and the sacrum in pregnant women, as well as balance the pelvic muscles. This in-turn removes torsion on the woman’s uterus, relieves the constraint on the baby and allows the baby to get into an optimal position for delivery. The World Health Organization states that no area should have higher than a 10-15% c-section rate. Currently the average rate in the United States is 30%, with some hospitals even higher! By helping the baby get into the optimal position and preventing breech position the Webster Technique is an excellent tool to help decrease the c-section rate. Currently the International Chiropractic Pediatric Association (ICPA) has the only database of Webster Technique certified chiropractors. You can visit their website at ICPA4kids.org. It is important to not wait until there is a problem to seek care. Chiropractic care throughout pregnancy can help to maintain normal spinal alignment and allow for the best pregnancy possible. Posture Changes During Pregnancy Pregnancy should be a time of joy for expectant mothers. Sometimes due to postural changes during pregnancy a women can experience discomfort and pain. Your lower back should normally have a slight curve in it. As the women’s belly grows more weight is distributed to the front of her body and that curve increases significantly. The abdominal muscles also stretch and weaken which allow for the low back curve to increase. An increase in the low back curve puts a lot of pressure on the posterior joints and ligaments of the spine. This also causes the women to bring her head and shoulders forward to try and compensate for the increased lower back curve. The increased breast size and weight will also cause a woman to bring her head and shoulders forward. When shoulders are rounded forward this can cause headaches, make breathing more difficult as well as digestion. Pregnant women also have a higher degree of ligament laxity. This is normal and allows the pelvis to open as the baby passes through the birth canal. However, this higher degree of ligament laxity can cause joints to become hypermobile and thus causes pain. Posture of the lower extremities also changes. In order to be able to stand upright with the weight of her growing belly, the pregnant women will tend to push her knees back into a hyperextended position. This can cause a lot of stress on the knee joints. The feet also tend to become flatter, so the woman has a broader base to stand on and carry the additional weight. Posture changes are inevitable during pregnancy, but there are some things you can do to help limit the consequences from this change of posture. •Don’t wear high heels. This will increase your low back curve even more • Consider wearing a pregnancy belt • Keep your abdominals and low back contracted, keeping your buttock tucked • Don’t cross your legs when sitting– this decreases circulation • Avoid slouching when sitting • Sit so your knees are level with your hips • When laying on your side, place a pillow between your knees and under your abdomen • If you have a young child– switch which hip you carry them on, this is also for laundry or groceries. By switching sides you will help to keep your pelvis and low back aligned. • Exercise– only with the approval of your physician • Chiropractic care Chiropractic care can not only help with aches and pain of pregnancy due to postural changes but it also helps to keep the pelvis aligned, which is very important for the actual birth of the child. Husband & wife team Drs. Brian and Lindsey own Complete Chiropractic in Wescosville and treat infants through seniors. Dr. Lindsey has advanced certifications in pediatrics and is certified in the Webster Technique. Dr. Brian has a special interest in treating athletes and specializes in soft tissue treatments like myofascial release and trigger point therapy. Their office is located at 5930 Hamilton Blvd #8, Allentown, Pa 18106, and you may reach them by telephone at (610)841-2204. They also accept many health insurance plans. www.completechirocenter.com When C contacted me recently announcing her pregnancy, I was thrilled and excited! I attended her last child's birth, and had gotten to know her over the past few years. Having boys at home, they were feeling especially blessed to be pregnant with a little girl. It was discovered at one of her appointments that C's baby was frank breech (instead of being head down, babies buttocks are presenting at the cervix, typically with the feet up above by the head). She did not want a ceserean! Her doctor agreed that the baby could be born in this position. C was both happy and a little worried. She didn't want surgery, but did fear the unknown of a vaginal breech birth. Together we came up with some important questions to ask her doctor, which helped her to understand the process and know what to expect for this type of delivery. Closer to her estimated due date C had another ultrasound which determined the baby's position had changed. Little Sara had now turned so her feet were in front of the cervix, this is known as footling presentation. This type of breech birth was not recommended vaginally due to the fact that her dr. felt the risks of a vaginal birth were too great. During our early planning stages, C and I had discussed what a gentle family-centered ceserean is, and what that could mean for her. A gentle family centered ceserean allows parents to choose many aspects of the birth; this could include dimmed lights, music of their choice, immediate skin to skin and breast-feeding if possible, photography, delayed cord clamping, and participating in the delivery by having the birth described to her as it is happening. C and I revisited this, as she now knew that little Sara would need to be born by C-section. Plans were made for myself and her husband to both support her in the room prior to the birth, and I would go back with her to the OR. C picked out a special CD to listen to during the birth. The doctors were respectful and didn't talk loudly about things unrelated to her birth. They described what was happening to both her and I. I massaged her temples, stroked her face, and held her hand. I took photos of the whole birth. The drape was lowered so C could participate in her baby's entrance earthside. The dr. delayed cord clamping & cutting. Sara was quickly evaluated by the nurses, and dressed warmly, because the OR was chilly. C was able to snuggle her for several minutes. C's husband came in the operating room with us to meet his baby and then followed her to the nursery afterwards. He even did skin to skin with her! The hospital staff was very respectful of C's desire to keep her placenta, and I encapsulated it for her for postpartum mood support. We also did a tincture, an umbilical cord keep sake, and placenta art prints. C had not wanted a ceserean, but because she planned for it, she was at peace. Because she was an active participant in her care, alongside her doctor, she felt supported. Knowing she had options and being able to choose the aspects of her care were really important to C. Many parents might feel that Doula support during a C-section is unwarranted, but in this birth story, it is evident that support is beneficial no matter the type of birth one plans for or ultimately has. Both C and her husband were thankful to have a doula by their side. We continue to support CL and her family during her postpartum stage, or fourth trimester. Help with breast-feeding, newborn care, and being available to answer questions several weeks after delivery helps foster confident mothers, which ultimately leads to a healthier and happier postpartum. If you have any questions regarding breech vaginal birth, family centered ceserean, creating a birth plan, or just want to know more about what doulas do, don't hesitate to contact us!
I live in Forks twps., with my husband and three children. I have 12 years of experience in the medical field, but after having very difficult pregnancies and the loss of our second child to stillbirth, I feel my life has taken me to different path. Because of this, I have chosen to train with Still Birthday. I deeply believe pregnancy, labor and birth are an amazing experience, whether it is complicated or not it can and should be amazing! I myself have had three emergency cesareans and a vbac. I specialize in emergency cesareans, NICU and loss during pregnancy, as all I have experienced first-hand. I am also current with BBP (Bloodborne Pathogens) certification for placental encapsulation. I have plans to study to be a Postpartum Doula and obtain my Breastfeeding Educator Certification (BEC).
Jackie has been mentoring with me for several weeks now. We actually met a few years ago over a mutual love for cloth diapers! I'm glad to be working with her and excited to see her take off into the birth world. If you have any questions for Jackie or want to meet with her for a consultation you can send her a message HERE. Many families who wish to labor naturally, and without drugs, do hire a birth doula. A birth doula offers prenatal education on comfort measures and breathing techniques for pain relief, and hands-on support during contractions, so it's no wonder women desire their support! A birth doula not only supports the laboring woman, but also their partner. As birth doulas, we have shown partners how to do foot massage during labor, and the couple how to use a rebozo and birth ball for pain relief.
But - birth doulas are not just for drug-free vaginal births. Many women who know they will require a c-section, or opt for one for personal reasons, choose to hire doulas, too. We work with our clients to plan family centered cesareans, hire birth photographers, and postpartum doulas. One of the most fulfilling rewards of being a birth doula is seeing a family feeling totally empowered at this new knowledge they have gained. Birth doulas support the whole family, no matter what type of birth they desire, or ultimately have. Natural Childbirth in the Hospital? Planned Cesarean? Home Waterbirth? Your body, your birth, your baby.....motherbaby|naturals Doulas support YOUR perfect birth! |
AuthorKiera talks about birth& babies& bonding! Archives
July 2017
Categories |
Fully Insured.
Areas We Serve:
Allentown, Bath, Bethlehem, Bethlehem Township, Catasaqua, Center Valley, Easton, Fogelsville, Forks, Fullerton, Hellertown, Lehigh Valley, Macungie, Nazareth, Northampton, Palmerton, Red Hill, Richland, Quakertown, Reading, Saucon Valley, Saylorsburg, Slatington, Whitehall and surrounding areas.
Hospitals: Doylestown, Geissinger, Lehigh Valley Hospital, Sacred Heart Allentown, St. Luke's Allentown & Bethlehem and surrounding hospitals.
We also serve HomeBirth and BirthCenter clients.
Areas We Serve:
Allentown, Bath, Bethlehem, Bethlehem Township, Catasaqua, Center Valley, Easton, Fogelsville, Forks, Fullerton, Hellertown, Lehigh Valley, Macungie, Nazareth, Northampton, Palmerton, Red Hill, Richland, Quakertown, Reading, Saucon Valley, Saylorsburg, Slatington, Whitehall and surrounding areas.
Hospitals: Doylestown, Geissinger, Lehigh Valley Hospital, Sacred Heart Allentown, St. Luke's Allentown & Bethlehem and surrounding hospitals.
We also serve HomeBirth and BirthCenter clients.












 RSS Feed
RSS Feed